Mental health care for all: let’s make it a reality!

Presently, the entire humanity is grappling with the COVID-19 pandemic, which has impacted the mental health of millions of people. Some groups, including health and other frontline workers, students, people living alone, and those with pre-existing mental health conditions, have been particularly affected. The levels of anxiety, fear, isolation, social distancing and emotional distress that is associated with the virus have become widespread as the world struggles to bring COVID-19 under control. Even the services for mental, neurological and substance use disorders have been significantly disrupted.
Then there is always a silver lining amidst the dark clouds. During the World Health Assembly in May 2021, governments from around the world recognized the need to scale up quality mental health services at all levels. And some countries have found new ways of providing mental health care to their populations.

Mental health is an integral part of health; it is more than the absence of mental illnesses. It is the foundation for well-being and effective functioning of individuals. It includes mental well-being, prevention of mental disorders, treatment and rehabilitation.
Determinants of mental health include individual attributes such as the ability to manage one’s thoughts, emotions, behaviours and interactions with others. In addition, social, cultural, economic, political and environmental factors have a role to play as do specific psychological and personality, and genetic factors.

Raising awareness and mobilizing efforts in support of mental health is necessary for addressing the situation.
World Mental Health Day is observed on 10th October every year, with the overall objective of raising awareness of mental health related issues around the world and mobilizing efforts in support of it. This Day provides an opportunity for all stakeholders working on mental health issues to talk about their work, and highlight gap areas in making mental health care a reality for people globally.
Mental health promotion involves creating an environment, which promotes healthy living and encourages people to adopt healthy lifestyle. Enabling environment through national mental health policies and legal frameworks are imperative for effective management of mental health disorders and providing overarching directions for ensuring mental health promotion. This calls for a multi-sectoral engagement and a life-course approach.
Treatment of mental health disorders is of utmost importance. It calls for comprehensive strategies for promotion, prevention, treatment and recovery through a whole-of-government approach. Policy makers should be encouraged to promote availability of and access to cost-effective treatment of common mental disorders at the primary health care level.
In India, mental illness is often followed by denial and hesitation to seek help and these statistics show the burden of mental disorders in our country. There’s still stigma attached to mental illnesses and the number of psychiatrists and counsellors in the country remain at an abysmal number.
Some statistics about Mental Health in India, as mentioned hereunder, shows the country has a long way ahead:
1. The mental health workforce in India has an acute shortage of psychiatrists and psychologists in comparison to the number of people suffering from mental health issues. (In India there are merely 0.3 psychiatrists, 0.12 nurses, 0.07 psychologists, and 0.7 social workers per 100,000 populations, according to World Health Organization)
2. WHO also estimates that about 7.5 percent Indians suffer from some mental disorder; 56 million Indians who suffer from depression and another 38 million Indians suffer from anxiety disorders.
3. Lancet studies suggest that India’s contribution to global suicide deaths increased from 25·3% in 1990 to 36·6% in 2016 among women, and from 18·7% to 24·3% among men. According to the National Mental Health Survey 2015-16 conducted by the National Institute of Mental Health & Neurosciences (NIMHANS), Bengaluru, under the purview of the Union Ministry of Health and Family Welfare, it was revealed that 9.8 million teenagers in the age group 13-17 years suffer depression and other mental health disorders and are “in dire need of active intervention”. Whereas, according to a study by the Lancet, suicide deaths ranked first among all causes of death in women aged 15-29 years.
4. According to World Health Organisation, the burden of mental health problems of the disability-adjusted life years per 100,000 populations is to the tune of 2,443, and of the age-adjusted suicide rate it is 21.1.
5. The Global Burden of Disease Study 1990–2017 conducted across the states of India shows – one in every seven Indians being affected by mental disorders of varying severity in 2017 and the proportional contribution of mental disorders to the total disease burden in India has almost doubled since 1990.
6. It is estimated that in India, the economic loss, due to mental health conditions, is going to be the USD 1.03 trillions, during the 2012 – 2030 period (WHO).
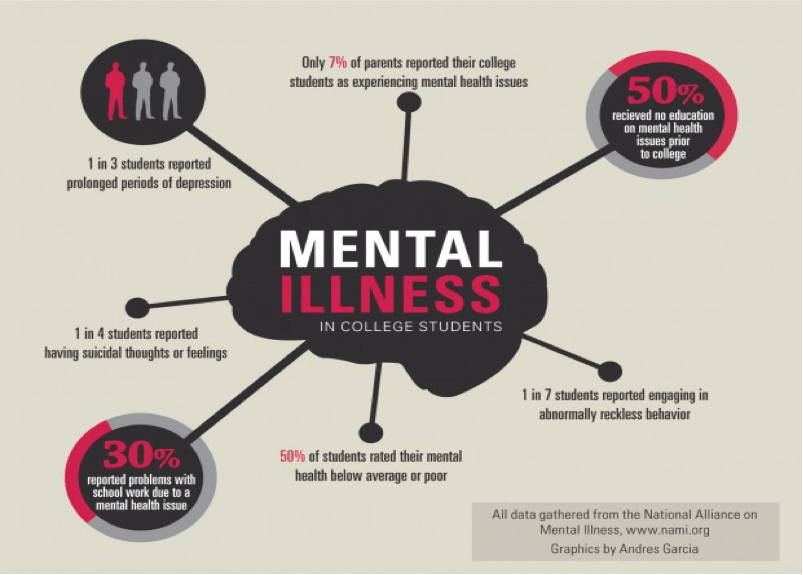
When it comes to person’s physical health, people are so conscious and aware these days – they have also access to a lot more things to maintain their health, they know everything about super-foods, the latest diet trends or workouts, but when it comes to mental health, the awareness just isn’t there. So many people aren’t even aware that they may be suffering from form of mental health issues and these statistics show the grim reality.
To address the huge burden of mental disorders and shortage of qualified professionals in the field of mental health, Government of India has been implementing National Mental Health Program (NMHP) since 1982. The district Mental Health Program was added to the Program in 1996. The Program was re-strategized in 2003 to include two schemes, viz. Modernization of State Mental Hospitals and Up-gradation of Psychiatric Wings of Medical Colleges/General Hospitals. The Manpower development scheme (Scheme-A & B) became part of the Program in 2009.
The objectives of National Mental Health Program (NMHP) include;
- To ensure the availability and accessibility of minimum mental healthcare for all in the foreseeable future;
- To encourage the application of mental health knowledge in general healthcare and in social development;
- To promote community participation in the mental health service development;
- To enhance human resource in mental health sub-specialties.
The COVID 19 pandemic has further highlighted the effects of inequality on health outcomes and no nation, however rich, has been fully prepared for this. The pandemic has and will continue to affect people, of all ages, in many ways: through infection and illness, sometimes resulting in death bringing bereavement to surviving family members; through the economic impact, with job losses and continued job insecurity; and with the physical distancing that can lead to social isolation.
We need to act, and act urgently!
Discover more from Vigyan Setu Foundation
Subscribe to get the latest posts sent to your email.




World health day
LikeLike
💐Happy mental health day to all of you 💐
LikeLike
💐Happy mental health day to all of you 💐
LikeLike
Happy mental health day too all of you
LikeLike
Happy mental health day 👍👍👍👍👍
LikeLike
World Mental Health Day
LikeLike
🎉🎉🎉🎉🎉🎉🎉🎉🎉🎉🎉🎉🎉🎉Happy mental Health day to all of you
👍🏻👍👍👍🌹🌹🌹🌹🌹🌹🌹🌹🌹🌹
LikeLike
Happy mental health day all of you
LikeLike
Happy mental health day too all of you
LikeLike
Happy mentel health day🎉🎉🎊🎊
LikeLike