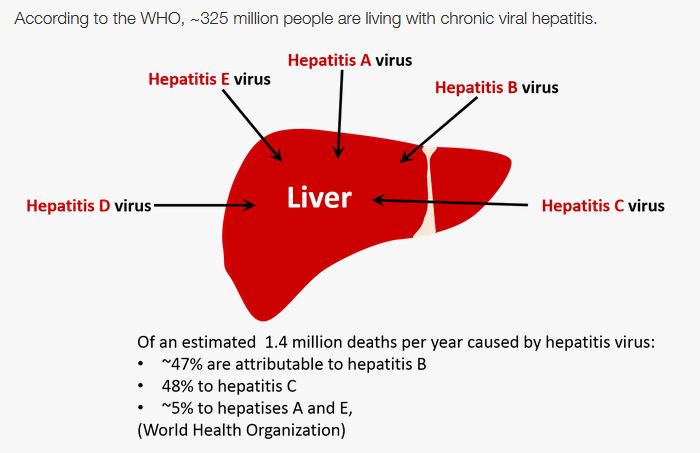
World Hepatitis Day (WHD) is globally celebrated on 28 July, as an opportunity to step up national and international efforts on hepatitis, encourage actions and engagement by individuals, partners and the public and highlight the need for a greater global response as outlined in the WHO’s Global hepatitis report of 2017.
The date of 28 July was chosen because it is the birthday of Nobel-prize winning scientist Dr Baruch Blumberg, who discovered hepatitis B virus (HBV) and developed a diagnostic test and vaccine for the virus.
WHD is a day for the world’s hepatitis community to unite and make the voices heard. It is a day to celebrate the progress made and to meet the current challenges. It is also an opportunity to increase awareness and encourage a real political change to jointly facilitate prevention, diagnosis and treatment. It is to raise awareness of the global burden of viral hepatitis and to influence real change. WHD is a great opportunity to raise awareness of the importance of knowing one’s own hepatitis status and to spread the word about treatment. Low coverage of testing and treatment is the most important gap to be addressed in order to achieve the global elimination goals by 2030.
Hepatitis is an inflammation of the liver It can occur due to a variety of factors, but the most common cause is a virus infection. Hepatitis can be acute (short-term) or chronic (long-term) and can have fatal complications.
The liver present in the right upper part of the abdomen serves several important functions, including:
- Metabolization of carbohydrates, fats, proteins, and drugs
- Storage of sugars, vitamins, and minerals
- Synthesis of certain proteins like albumin and blood clotting factors
- Production of bile for digestion of fats
- Activation of enzymes required for body functions
General causes of hepatitis:
- Virus and other infections
- Alcohol
- Drugs
- Toxins
- Autoimmune response (the body’s immune system attacks its own tissues)
- Ischemia (decreased oxygenation of the liver)
- Metabolic disorders
Viral Hepatitis is an inflammation of the liver caused by a viral infection. There are five main hepatitis viruses, referred to as types A, B, C, D and E. These five types are of greatest concern because of the burden of illness and death they cause and the potential for outbreaks and epidemic spread.
Hepatitis A:
Vaccine: Yes
Treatment: Yes
Cure: Most people make a full recovery
Hepatitis A virus (HAV) primarily spreads when an uninfected (and unvaccinated) person ingests food or water that is contaminated with the faeces of an infected person. The disease is closely associated with unsafe water or food, inadequate sanitation, poor personal hygiene and oral-anal sex.
Symptoms of hepatitis A range from mild to severe and can include fever, malaise, loss of appetite, diarrhoea, nausea, abdominal discomfort, dark-coloured urine and jaundice (a yellowing of the eyes and skin). Not everyone who is infected will have all the symptoms.
Improved sanitation, food safety and immunization are the most effective ways to combat hepatitis A.
The spread of hepatitis A can be reduced by:
- adequate supplies of safe drinking water;
- proper disposal of sewage within communities; and
- personal hygiene practices such as regular handwashing before meals and after going to the bathroom.
Hepatitis B:
Vaccine: Yes
Treatment: Yes
Cure: In development
Hepatitis B is a potentially life-threatening liver infection caused by the hepatitis B virus (HBV). It is a major global health problem. It can cause chronic infection and puts people at high risk of death from cirrhosis and liver cancer.
Hepatitis B is most commonly spread from mother to child at birth (perinatal transmission) or through horizontal transmission (exposure to infected blood). The development of chronic infection is common in infants infected from their mothers or before the age of 5 years.
Hepatitis B is also spread by needlestick injury, tattooing, piercing and exposure to infected blood and body fluids, such as saliva and menstrual, vaginal and seminal fluids. Transmission of the virus may also occur through the reuse of contaminated needles and syringes or sharp objects either in health care settings, in the community or among persons who inject drugs. Sexual transmission is more prevalent in unvaccinated persons with multiple sexual partners.
In addition to infant vaccination, WHO recommends the use of antiviral prophylaxis for the prevention of hepatitis B transmission from mother-to-child. Implementation of blood safety strategies and safer sex practices, including minimizing the number of partners and using barrier protective measures (condoms), also protect against transmission.
Hepatitis C:
Vaccine: No
Treatment: Yes
Cure: Yes
Hepatitis C virus (HCV) causes both acute and chronic infection. The hepatitis C virus is a bloodborne virus. It is most commonly transmitted through:
- the reuse or inadequate sterilization of medical equipment, especially syringes and needles in healthcare settings;
- the transfusion of unscreened blood and blood products; and
- injecting drug use through the sharing of injection equipment.
HCV can be passed from an infected mother to her baby and via sexual practices that lead to exposure to blood (for example, people with multiple sexual partners and among men who have sex with men); however, these modes of transmission are less common.
Those who are acutely symptomatic may exhibit fever, fatigue, decreased appetite, nausea, vomiting, abdominal pain, dark urine, pale faeces, joint pain and jaundice (yellowing of skin and the whites of the eyes).
Primary prevention interventions recommended by WHO include:
- safe and appropriate use of health care injections;
- safe handling and disposal of sharps and waste;
- provision of comprehensive harm-reduction services to people who inject drugs;
- testing of donated blood for HBV and HCV (as well as HIV and syphilis);
- training of health personnel; and
- prevention of exposure to blood during sex.
Hepatitis D:
Vaccine: No (although hepatitis D only affects people living with hepatitis B which there is a vaccine for)
Treatment: Yes
Cure: No
Hepatitis D is caused by the hepatitis D virus (HDV), which requires HBV for its replication. Hepatitis D infection cannot occur in the absence of hepatitis B virus. HDV-HBV co-infection is considered the most severe form of chronic viral hepatitis due to more rapid progression towards hepatocellular carcinoma and liver-related death.
The routes of HDV transmission, like HBV, occur through broken skin (via injection, tattooing etc.) or through contact with infected blood or blood products. Transmission from mother to child is possible but rare. Vaccination against HBV prevents HDV coinfection and hence expansion of childhood HBV immunization programmes has resulted in a decline in hepatitis D incidence worldwide.
In acute hepatitis, simultaneous infection with HBV and HDV can lead to a mild-to-severe hepatitis with signs and symptoms of indistinguishable from those of other types of acute viral hepatitis infections. These include fever, fatigue, loss of appetite, nausea, vomiting, dark urine, pale-coloured stools and jaundice (yellow eyes).
While WHO does not have specific recommendations on hepatitis D, prevention of HBV transmission through hepatitis B immunization, including a timely birth dose, additional antiviral prophylaxis for eligible pregnant women, blood safety, safe injection practices in health care settings and harm reduction services with clean needles and syringes are effective in preventing HDV transmission. Hepatitis B immunization does not provide protection against HDV for those already infected with HBV.
Hepatitis E:
Vaccine: No
Treatment: Yes
Cure: Most people make a full recovery
Hepatitis E is inflammation of the liver caused by the hepatitis E virus (HEV).
The virus is shed in the stools of infected persons and enters the human body through the intestine. It is transmitted mainly through contaminated drinking water. The infection is usually self-limiting and resolves within 2–6 weeks. Occasionally a serious disease known as fulminant hepatitis (acute liver failure) develops, which can be fatal.
Hepatitis E infection is found worldwide and is common in low- and middle-income countries with limited access to essential water, sanitation, hygiene and health services. In these areas, the disease occurs both as outbreaks and as sporadic cases. The outbreaks usually follow periods of faecal contamination of drinking water supplies and may affect several hundred to several thousand persons. Some of these outbreaks have occurred in areas of conflict and humanitarian emergencies such as war zones and camps for refugees or internally displaced populations, where sanitation and safe water supply pose special challenges.
Typical signs and symptoms of hepatitis include:
- an initial phase of mild fever, reduced appetite (anorexia), nausea and vomiting lasting for a few days;
- abdominal pain, itching, skin rash, or joint pain;
- jaundice (yellow colour of the skin), dark urine and pale stools; and
- a slightly enlarged, tender liver (hepatomegaly).
Prevention is the most effective approach against the infection. At the population level, transmission of HEV and hepatitis E infection can be reduced by:
- maintaining quality standards for public water supplies; and
- establishing proper disposal systems for human faeces.
On an individual level, infection risk can be reduced by:
- maintaining hygienic practices; and
- avoiding consumption of water and ice of unknown purity.

Discover more from Vigyan Setu Foundation
Subscribe to get the latest posts sent to your email.